Advanced Spine Surgery · Naples & Fort Myers, FL
The Modern
Discectomy
A multi-step surgical protocol combining minimally invasive METRx tube technology, optional Barricaid annular repair, and optional PRP biologic therapy — engineered to remove your herniated disc, reduce reherniation risk, and get you back to life fast.
"Disc surgery has evolved. Patients deserve every tool available — not just a basic discectomy, but a complete biological repair."
Dr. G. Katsevman, MD · Fellowship-Trained, Barrow Neurological Institute18mm METRx tube
day of surgery
at 6 weeks post-op
risk with Barricaid
Who benefits
Are you a candidate for The Modern Discectomy?
This procedure is designed for patients with a confirmed lumbar disc herniation causing leg pain, sciatica, numbness, or weakness who have not found lasting relief from conservative care.
Sciatica or Leg Pain
Sharp, shooting, or burning pain radiating from the lower back into the buttock, leg, or foot — often worse with sitting, coughing, or bending forward.
Confirmed Disc Herniation
MRI-confirmed herniated or extruded disc pressing on a nerve root. L4-5 and L5-S1 are the most common levels treated.
Failed Conservative Care
Physical therapy, medications, or injections have not provided lasting relief — or symptoms are severe enough to warrant surgical evaluation.
Reherniation Risk
Patients with a large annular defect face higher reherniation risk. When present and indicated, Barricaid seals the defect at the time of surgery.
The procedure
One surgery. Multiple layers of protection.
Each element is independently proven. Combined, they represent the most advanced approach to lumbar disc herniation surgery available in Southwest Florida.
Minimally Invasive Tubular Discectomy
Traditional open discectomy requires cutting and retracting the large muscles of the back — causing significant tissue damage, more post-operative pain, and a longer recovery. Dr. Katsevman performs a fully minimally invasive discectomy through an 18mm METRx working channel, an incision smaller than a quarter.
The tube is dilated gently between muscle fibers rather than cutting through them, dramatically reducing trauma to surrounding tissue. A high-definition microscope gives Dr. Katsevman a magnified view of the nerve and disc fragment, which is then carefully removed to fully decompress the nerve root.
Patients walk the same day as surgery and go home the same day — no overnight stay. There are no activity restrictions at six weeks post-operatively.
Annular Defect Repair — Reducing Reherniation Risk
When a disc herniates, it tears through the outer disc wall — the annulus fibrosus. After the herniated fragment is removed, this tear (the annular defect) remains open. Patients with a large defect are at significantly higher risk of the remaining disc material re-pushing through that same opening.
When the defect meets clinical criteria, Dr. Katsevman implants the Barricaid® Annular Closure Device — a small, bone-anchored woven implant that permanently seals the defect through the same incision. Clinical studies show Barricaid significantly reduces reherniation risk and reoperation rates compared to discectomy alone.
Not every patient qualifies. Eligibility is evaluated before surgery and confirmed intraoperatively. When indicated, it is one of the most impactful additions available.
PRP Therapy — Accelerating Your Healing
At the conclusion of surgery, Dr. Katsevman can apply Platelet-Rich Plasma (PRP) — a concentration of your body's own growth factors prepared from a small blood draw before surgery. PRP delivers a powerful healing signal at precisely the moment your body needs it most.
PRP is delivered to three targeted locations:
Into the disc space — to support disc biology and promote healing at the annular repair site.
Into the epidural space — to bathe the decompressed nerve root in growth factors, reducing inflammation and facilitating nerve recovery.
Into the surgical incision — to promote soft-tissue healing and minimize scar formation.
PRP comes entirely from your own blood — no synthetic additives, essentially no allergy risk. Because it is currently off-label for spine surgery, PRP is typically not covered by insurance and is offered as a patient-elected add-on.
How it compares
Traditional discectomy vs. The Modern Discectomy
Standard / Traditional Discectomy
Large incision (1–3 inches)Requires cutting and retracting back muscles to access the disc.
Significant muscle disruptionRetraction causes damage, more pain, and a longer recovery.
Annular defect left openDisc wall tear remains unsealed — a pathway for reherniation stays open.
No biologic supportRecovery relies on baseline healing — no augmentation available.
Prolonged activity restrictionsOften involves weeks of limitations on bending, lifting, and movement.
Higher reherniation rateWithout annular closure, a significant percentage of patients re-herniate within 2 years.
The Modern Discectomy · Dr. Katsevman
Incision smaller than a quarter18mm METRx tube provides full surgical access through a tiny opening.
Muscle-sparing techniqueTube dilates between fibers — no cutting, less pain, faster return to activity.
Barricaid seals the defect (if indicated)Bone-anchored implant permanently closes the annular tear when present.
Optional PRP augmentationGrowth factors target the disc, nerve, and incision for accelerated healing.
Walk same day · home same dayNo activity restrictions at 6 weeks post-operatively.
Reduced reherniation riskBarricaid significantly lowers re-herniation likelihood and reoperation rates.
Common questions
What patients ask most
What is recovery like after this surgery? +
Patients walk the same day as surgery and go home the same day — there is no overnight hospital stay. Most patients return to desk work within 1–2 weeks. At six weeks post-operatively, there are no activity restrictions. The minimally invasive tube approach causes far less muscle trauma than traditional open surgery, which is the primary driver of this rapid recovery.
Does everyone get the Barricaid device? +
No — Barricaid is indicated only for patients who meet specific clinical criteria, primarily those with a large annular defect confirmed during surgery. Dr. Katsevman evaluates eligibility before the procedure and makes the final determination intraoperatively. Not every herniation produces a qualifying defect, but when it does, Barricaid is one of the most impactful tools available to reduce the risk of reherniation.
Is PRP required, and does insurance cover it? +
PRP is completely optional — it is offered as a patient-elected add-on for those who want to pursue every available advantage in their recovery. Because PRP is currently off-label for spine surgery, it is typically not covered by insurance. The core discectomy is covered by most major insurance plans when medically indicated, and Barricaid coverage varies by insurer and plan. Our team will walk you through all cost details at your consultation.
Will insurance cover this procedure? +
The minimally invasive discectomy is covered by most major insurance plans when medically indicated. We work with all insurance plans — even if we are out of network, we can often utilize out-of-network benefits or pursue a GAP exception when surgery is part of your treatment plan. Our team will guide you through your specific options before any decisions are made.
Can I get a second opinion if I've already been told I need surgery? +
Absolutely — and Dr. Katsevman actively encourages it. A second opinion is one of the most important steps before any spine procedure. He offers in-person and telemedicine second-opinion consultations for patients across Florida and nationally. Bring your MRI images and prior records. Many patients find their surgical plan can be meaningfully refined after a second look.
What spine levels can be treated this way? +
The Modern Discectomy is primarily designed for lumbar (lower back) disc herniations — most commonly L4-5 and L5-S1, the levels responsible for the vast majority of sciatica cases. Dr. Katsevman also performs minimally invasive cervical (neck) disc surgery using a different approach. During your consultation he will review your imaging and determine the precise technique best suited to your anatomy and diagnosis.
"My goal is not just to remove your disc problem — it's to give your spine the best possible chance at a durable, lasting recovery."
Gennadiy (Gene) A. Katsevman, MD
Neurosurgeon & Minimally Invasive Spine Surgeon
Fellowship-trained at Barrow Neurological Institute under Dr. Juan Uribe — a world pioneer in minimally invasive spine surgery
Neurosurgery residency, West Virginia University — Level 1 Trauma Center
30+ peer-reviewed publications in spine surgery and neurosurgery
Naples Top Doctor in Neurosurgery — 2024, 2025, and 2026
5-star Google rating · Healthgrades Choice Provider · WebMD Preferred Provider
U.S. News & World Report Patients' Top Choice
Offices in Naples and Fort Myers · Telemedicine available nationwide
Take the next step
Ready to discuss your options?
Schedule a consultation with Dr. Katsevman in Naples or Fort Myers — or via telemedicine — to review your imaging and find out if The Modern Discectomy is right for you.
6101 Pine Ridge Road #101
Naples, FL 34119
Fort Myers, FL 33919
Available nationwide

METRX Minimally Invasive Tubes
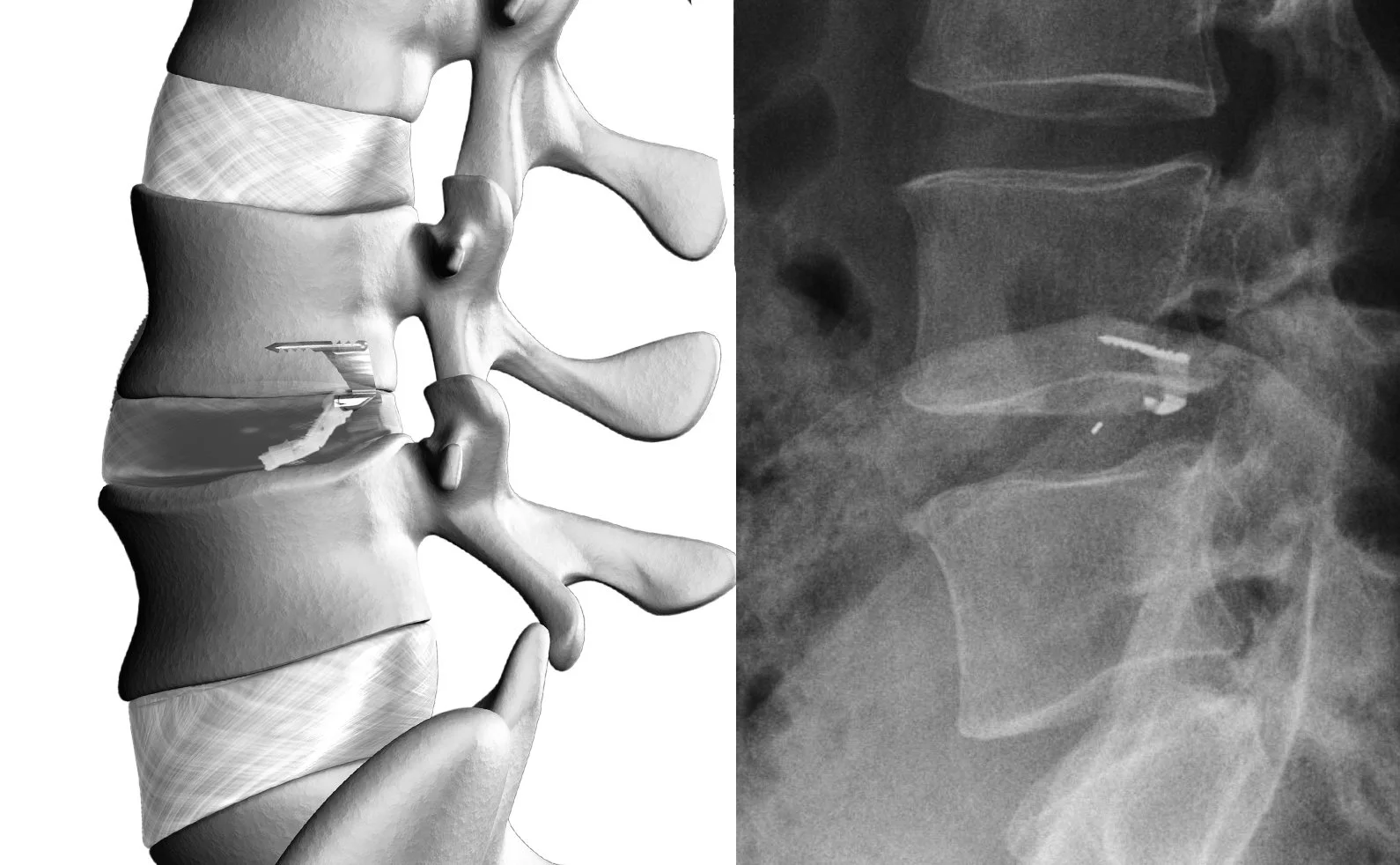
Barricaid Annular Closure Device

Platelet-Rich Plasma (PRP)
